However, from a research standpoint, it is likely important to enroll patients with more homogenous features, including medication history, in future studies. It is not certain to what degree structural factors might be affected by medication. Only one report included drug-naïve narcolepsy patients. In three studies, more than half of the patients were medicated for daytime sleepiness, and, in another two studies, medication history was not mentioned. Patients’ characteristics are quite variable between studies. However, brain regions showing decreased GMV or GMC across the studies are likely to be important in the development of narcolepsy. It is not clear whether GMV or GMC is more a more sensitive detection method for structural abnormalities in the brain. Optimized VBM can quantify GM differences between subjects both differences in the relative distribution of GMC and absolute differences in GMV. Four showed GMV changes and two reported GMC reductions in patients. There were differences in both methodology (the statistical parametric mapping version, modulated or unmodulated, grand mean scaling, absolute or relative thresholding, and sample size) and the composition of patients in the studies (the presence of cataplexy, disease duration, drug naivety, accompanying symptoms). It also suggested that the structural substrates showing decreased GMC might be responsible for wake-sleep controls, attention, or memory. Reduced GMC in the hypothalamus and nucleus accumbens supported the hypothesis that these reductions are associated with daytime sleepiness and cataplexy in narcolepsy patients. Small volume correction emphasized GMC reduction in the bilateral nucleus accumbens, hypothalami, and thalami ( Fig. The most recent study demonstrated reduced GMC in the bilateral thalami, left gyrus rectus, bilateral frontopolar gyri, bilateral short insular gyri, bilateral superior frontal gyri, and right superior temporal and left inferior temporal gyri in patients with narcolepsy compared to healthy controls ( Fig. Two studies showed decreases in GMV in the inferior temporal/frontal and right prefrontal/frontomesial regions, contributing to cognitive impairments, such as attentional deficits. They suggested that neuronal losses affected the hypothalamus and related hypocretinergic structures, as well as major sites of hypocretin projections and the nucleus accumbens. Two of studies showed decreases in GMC or GMV in the hypothalamus. :max_bytes(150000):strip_icc()/narcolepsy-symptoms-5111881_Final-86832b1d82564a39a4de1682ff57a1c0.jpg)
The initial study did not find any structural changes in narcoleptic patients however, most of studies reported significant decreases in gray matter volume (GMV) or concentration (GMC). There have been several VBM studies in patients with narcolepsy, but findings from this studies have been ambiguous. VBM visualizes between-group differences, statistical comparisons of tissue composition, and gray matter (GM) versus WM across all brain regions, with high-resolution scans. Abnormalities of brain structure can be investigated using more delicate and updated technologies such as voxel-based morphometry (VBM) in group analyses. Until now, it has been widely accepted that brain MRIs of individuals with idiopathic narcolepsy are normal by routine visual inspection. Another study, however, could not reproduce this finding. Keywords: Cataplexy Gray matter Magnetic resonance imaging Narcolepsy White matterĭecades ago, the first published neuroimaging paper reported an abnormality of the pontine reticular formation, where REM sleep is generated, in the brain MRIs of three idiopathic tic patients. Thus, structural neuroimaging may help clarify the underlying mechanism of certain phenotypes of narcolepsy syndrome. 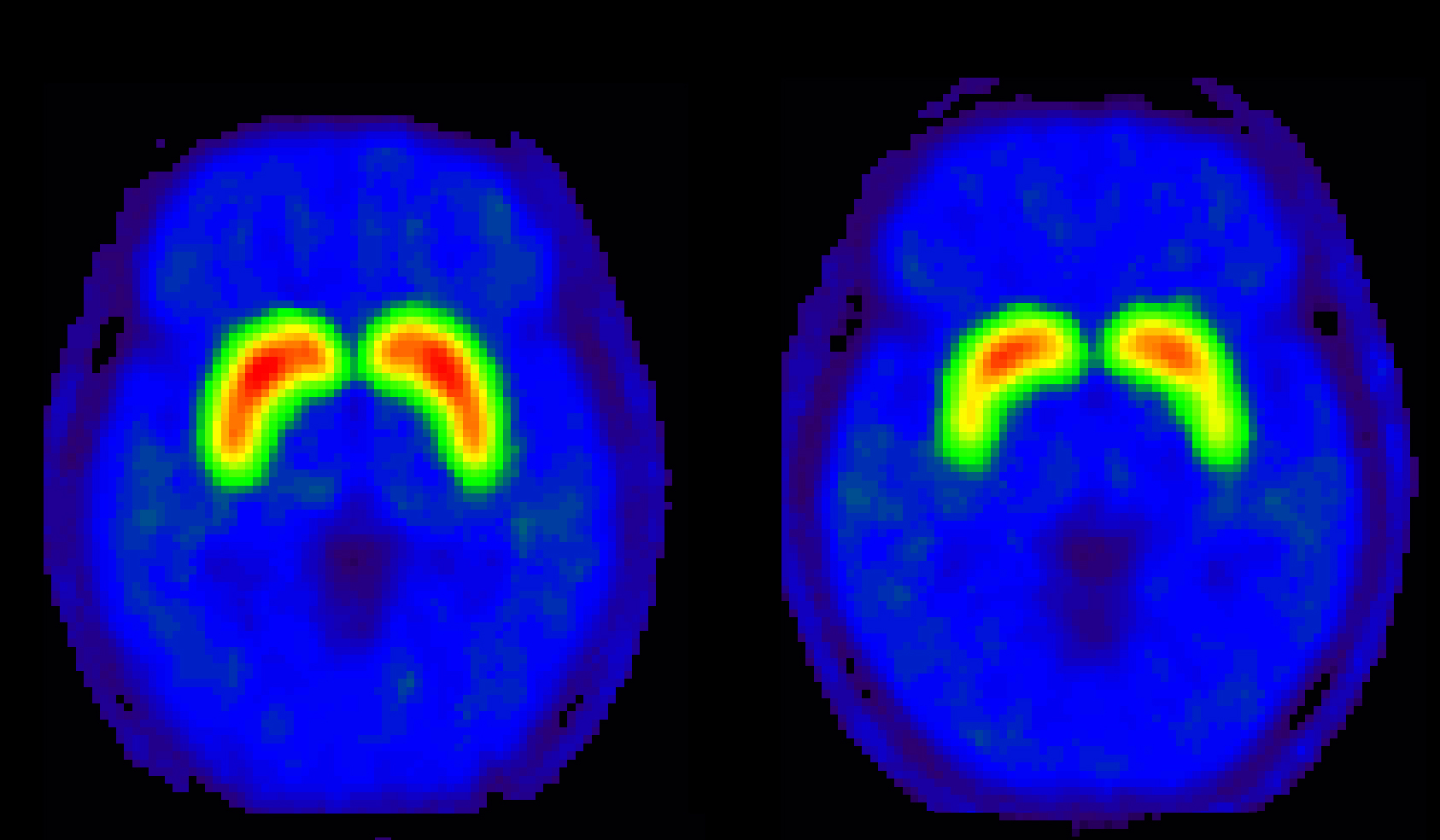
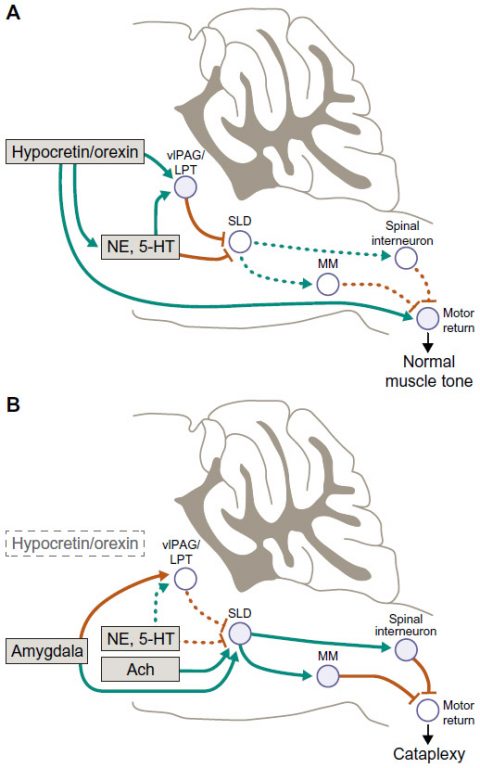
Longitudinal MRI data have suggested progression in narcolepsy, showing progressive corticalthinning in disease, and that such progression may become fasterin the case of patients with earlier disease onset. Numerous studies, exploring gray matter and white matter, showed distinct aspects of disease and symptoms in narcolepsy with cataplexy related to the hypothalamus, thalamus, amygdalo-hippocampus, and frontoparietal cortex. Brain magnetic resonance imaging (MRI) studies, in particular, demonstrated distinct structural changes in multiple brain areas of patients with narcolepsy. Developments in neuroimaging techniques have advanced the understanding and characterization of the pathophysiology of this disease. Narcolepsy is a chronic neurological disorder associated with abnormal regulation of the sleep-wake cycle, resulting in excessive daytime sleepiness, disturbed nocturnal sleep, and rapid eye movement (REM) sleep phenomena including cataplexy. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
